What is glucagon and how can a glucagon kit help someone with diabetes?
Medically reviewed by Dr Sultan Linjawi, Endocrinologist & Diabetes Specialist — January 2026

Find the Right Program for You
Select the situation that best describes you
What is glucagon?
Glucagon is a hormone which is produced by the alpha cells of the pancreas. When blood glucose levels fall too low, glucagon raises the levels of glucose in the blood by converting stored glycogen in the liver to glucose.
Insulin is also hormone but is produced by the beta cells of the pancreas. The action of insulin is to decrease levels of glucose in the blood stream.
Glucagon’s effects are the opposite to insulin and both of these hormones work together to keep our blood glucose levels balanced and at a safe range.
What does glucagon do in the body? How does glucagon affect blood glucose levels?
Glucagon is released to stop blood glucose levels from becoming too low, the pancreas will release glucagon which can stimulate the liver to release glucose, giving our cells an important source of energy. Glucose and insulin are two hormones, released from the pancreas, that work together to keep our blood glucose levels in a safe range.
Glucagon can also be released by the pancreas when the body needs additional or extra glucose, for example during vigorous or intense exercise.
The action of glucagon includes to:
- Stimulate the liver to break down glycogen (the stored form of glucose) which can be released into the bloodstream as glucose
- Activate gluconeogenesis, which is the process of converting amino acids into glucose, which can also be used for energy. This process occurs when glucose stores become low
- Decrease fatty acid synthesis by breaking down stored fat from adipose tissue and the liver into free fatty acids, which can also be used as energy by the body’s cells when required
It’s important to note that glucose is the body’s preferred energy source.
Symptoms of low blood glucose levels
The symptoms of low blood glucose levels, also called hypoglycaemia, can vary from person to person. Low blood glucose levels is more common in people with diabetes. The symptoms of hypoglycaemia can be mild, for example sweating or feeling hungry, or they can be severe, for example passing out or fainting.
Early symptoms of hypoglycaemia include:
- sweating or shaking
- feeling hungry
- feeling worried
- light headedness
If left untreated, symptoms of hypoglycaemia can become serious. This includes:
- a headache, blurry vision, or feeling dizzy
- feeling weak or having trouble walking
- confusion or not thinking clearly
- passing out/ fainting
Risk factors for low blood glucose levels
There are some risk factors for hypoglycaemia. These include:
- Older age
- Longer duration of diabetes diagnosis
- Inconsistent meal timing, including missed meals and low carbohydrate meals
- History of hyperglycaemia, particularly a recent history of severe hypoglycaemia
- Exercise
- Alcohol consumption
How do I know if I have low blood glucose?
To be diagnosed with low blood glucose levels, you must exhibit symptoms of low blood glucose levels, as well as:
- have low blood glucose when you show symptoms
- feel better after eating or drinking something that can bring your blood glucose levels back to normal
Your doctor may perform some tests to confirm if you have low blood glucose levels, for example a blood test.
Ideal blood glucose levels
Blood glucose levels are measured in millimoles per litre of blood (mmol/L) or milligrams per decilitre of blood (mg/dL) depending on which area of the world you live in. Blood glucose level targets also differ depending on your age, how long you have had diabetes for, what types of medications you are taking, and if you have any other medical conditions in addition to diabetes. Your doctor will take off of this into consideration when determining what your blood glucose level targets are.
Normal blood glucose levels are between 4.0-7.8mmol/L or 72-140mg/dL.
| mmol/L | mg/dL | |
|---|---|---|
| Before meals | 4-8 mmol/L | 72-145 mg/dL |
| After meals | less than 10mmol/L | 180 mg/dL |
| mmol/L | mg/dL | |
|---|---|---|
| Before meals | 6-8 mmol/L | 106-145 mg/dL |
| After meals | 6-10mmol/L | 106-180 mg/dL |
Glucagon and diabetes – how does it help?
In people who have diabetes, glucagon can help to raise blood glucose levels when blood glucose levels become too low. However, glucagon may cause blood glucose levels to become too high and this may be caused by not enough insulin present to help glucose go from in the blood stream into the cells. This may be the case for people with type 2 diabetes as they are insulin resistant. In people with type 1 diabetes, high levels of insulin may inhibit the release and action of glucagon.
Glucagon kits – what are they?
Glucagon can be administered via an injection in response to an episode of severe hypoglycaemia.
Glucagon injection kits can be used to treat episodes of severe hypoglycaemia. These kits are designed to be used by a carer or family member of someone who has diabetes, who is unable to treat themselves during a hypoglycaemic event or oral treatment, i.e. jelly beans, has been unsuccessful.
Once injected, the glucagon is absorbed into the blood stream and travels to the liver where it can signal for the liver to release stored glucose (glycogen). Once glucose is released from the liver, it enters the bloodstream, raising your blood glucose levels. It can take approximately 10-15 minutes for blood glucose levels to rise back to a safe level.
How to use the glucagon kit
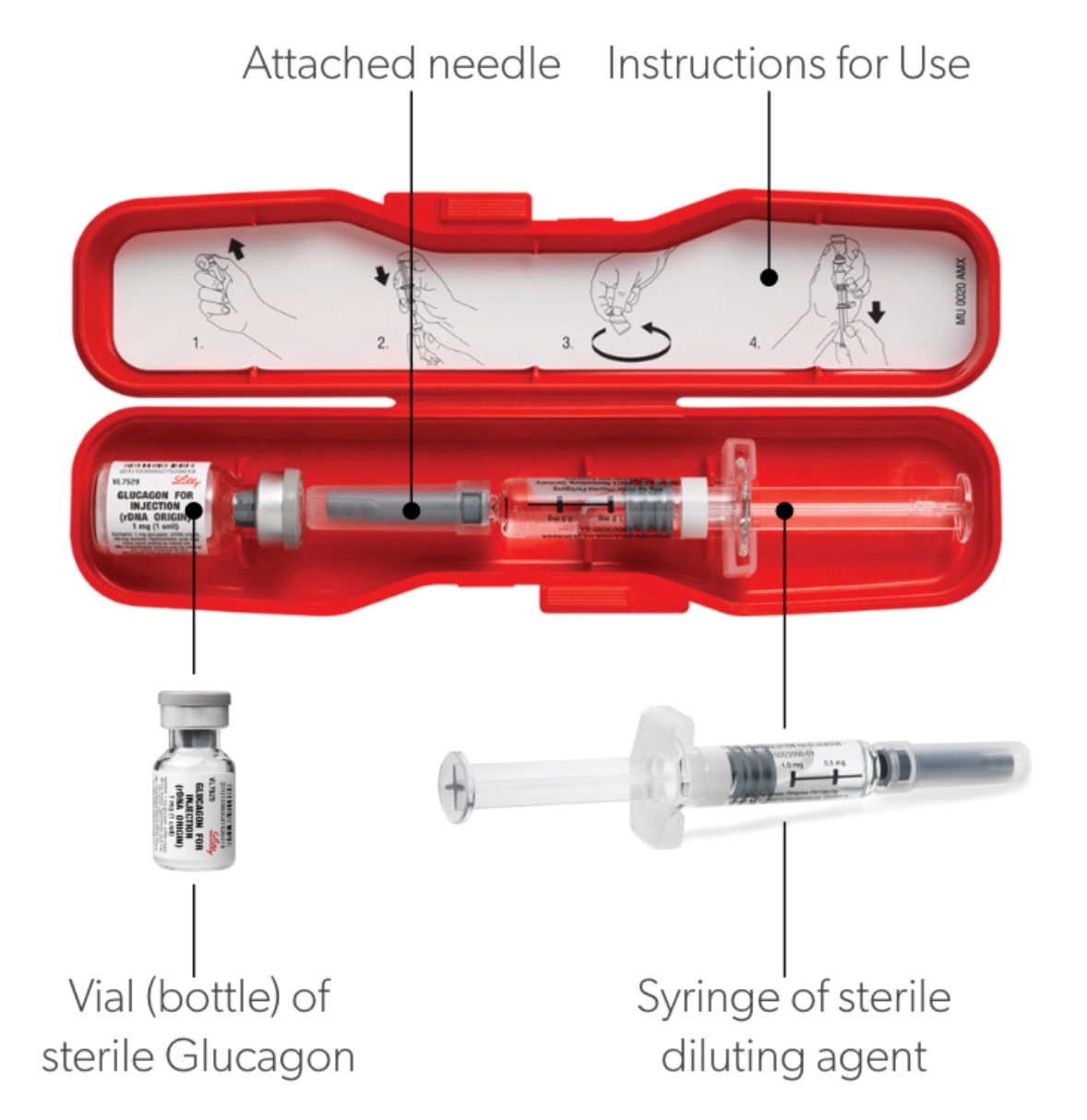
The glucagon kit comes with a syringe, and a vial of powder and a vial of liquid. There are instructions for how to mix the liquid and powder together within the kit. Before administering the glucagon injection, you should first put the person into the recovery position, where the person is laying on their side.
The basic instructions are as follows:
- Open the seal on the vial of glucagon powder.
- Remove the cap off of the syringe. Do not remove the plastic clip from the syringe. Removing the plastic clip can cause the rod to come out of the syringe.
- Insert the needle into the rubber stopper on the vial and inject the entire contents of the needle into the vial of glucagon powder until the syringe is empty, then remove the syringe from the vial.
- Gently swirl the vial to mix the liquid and powder, until the liquid becomes clear. The glucagon solution can only be used when the solution is clear and is a water-like consistency.
- Insert the syringe into the vial again and slowly withdraw all of the liquid.
- Clean the injection site (buttock, arm, or thigh) with an alcohol swap and inject the glucagon solution immediately after mixing. After withdrawing the needle, apply light pressure to the injection site.
- Keep the person on their side. When an unconscious person wakes, it’s important they’re on their side as they may vomit.
- Safely dispose of the syringe and vial.
Recovering from the glucagon injection
After a person recovers following a glucagon injection, try to feed them some fast-acting glucose, for example fruit juice, following by longer acting carbohydrates, for example fruit, bread, or crackers.
Where to keep glucagon kits?
It’s important to keep an emergency glucagon kit with your other diabetes supplies in case of an emergency. It’s a good idea to have more than emergency kit, for example having one on you while you’re away from home, as well as keeping some with close relatives or friends, or in places where you and your child spend a lot of time. If you keep any glucagon kits with friends, family, at school or work, make sure that other people know where the kits are and how to use them.
Some examples of where emergency glucagon kits can be kept include:
For children
- at school, for example the nurse’s office or administration office
- at the day care or childcare centre
- with a babysitter
- with a sporting coach
- at the home of relatives
For adults
- at the workplace
- at the homes of close friends and relatives
- with you when you’re travelling
- with a sporting coach
Looking for more diabetes videos?
Check out our latest diabetes videos for more content.