How is type 1 diabetes treated? Are there different types of insulin treatments?
Medically reviewed by Dr Sultan Linjawi, Endocrinologist & Diabetes Specialist — January 2026
In type 1 diabetes, treatment involves two key factors:
- Checking blood glucose levels regularly to make sure they aren’t too low or too high, and
- Using insulin (through a pen or pump) to help keep blood glucose levels in a safe range
What is insulin?
Insulin occurs naturally in the body and is produced by the pancreas. Diabetes is a disorder that affects the way the body uses glucose (also commonly referred to as sugar). For people with type 1 diabetes, the pancreas is unable to produce insulin which helps move glucose from the blood stream into the cells to be used for energy. If there is not enough insulin being produced, then it can lead to glucose building up in the blood, causing high blood glucose levels.
Insulin is the main treatment for people with type 1 diabetes. Insulin lowers the blood glucose level of a person with type 1 diabetes. Insulin can be delivered through injections that a person will give themselves or through an insulin pump.
Type 1 Diabetes Content |
|---|
| Type 1 Program |
| Overview |
| Risk Factors |
| Symptoms |
| Diagnosis |
| Complications |
| Treatment |
| Diet |
| Monitoring |
| Tools |
| Mental Health |
| Prevention |
Insulin therapy for type 1 diabetes
The goal of insulin therapy is to replace insulin that can’t be produced by the pancreas to achieve normal glucose. Since insulin is a crucial hormone that allows glucose in the blood stream to get into the muscle and fat cells, replacing insulin is necessary for people with type 1 diabetes.
There are many different types of insulin and can be classified by the onset and duration of action. These include:
- rapid acting insulin
- intermediate acting insulin
- long acting insulin
Many people with type 1 diabetes use 2 different types of insulin every day. This helps to ensure that the body has insulin all day and night.
Intensive insulin therapy can be delivered by either multiple daily injections (MDI) or through continuous insulin infusion (pump).
In the Diabetes Control and Complications Trial (DCCT), it was found that intensive therapy aimed at lower levels of blood glucose, resulted in decreased rates of retinopathy, neuropathy, and nephropathy in people with type 1 diabetes (The Effect of Intensive Treatment of Diabetes on the Development and Progression of Long-Term Complications in Insulin-Dependent Diabetes Mellitus). The DCCT study also found that ongoing blood glucose control (for a period of 6.5 years) has the lasting benefit of reducing cardiovascular morbidity and mortality in people with type 1 diabetes.
Choice of insulin delivery
The choice of insulin delivery is up to personal preference and can also depend on lifestyle and cost.
It has been found that glycaemic control is quite similar between multiple daily injections (MDI) and continuous subcutaneous insulin infusions (CSII), most commonly referred to as insulin pumps. Modern insulin pumps often have integrated continuous glucose monitoring systems, which can help to reduce hypoglycaemia during long periods without food, i.e. during sleep.
In the Diabetes Control and Complications Trial (DCCT), patients could choose between MDI or CSII for the duration of the trial. During the trial it was found that glycaemic control, frequency of severe hypoglycaemia, and progression of microvascular disease were similar across both types of insulin therapy.
Multiple daily injections
Multiple daily injections (MDI) requires a person to inject insulin over multiple times per day. It should be monitored through continuous glucose monitoring or self-monitoring of blood glucose levels through finger prick tests.
How do I give myself an insulin shot?
Prefilled insulin pens are a lot easier to use compared to the older style insulin syringes and insulin bottles. The insulin pens consist of the prefilled insulin cartridge, a needle, and knob which you can turn to mark the number of insulin units you need to take.
When using insulin, you will first need to determine how much insulin to use based. Once you have chosen the insulin unit, it is the simple process that you follow when injecting insulin:
- Attach a new needle tip to the pen
- Choose the part of your body where you will inject the insulin – this might be your abdomen, thigh, or the back of your arm
- Pinch the skin and quickly insert the needle
- Push down the plunger all the way and count to 5 – this is to make sure that all the insulin will be released from the pen
- Let go of the pinched skin and remove the pen
When disposing of the pen needles, make sure to dispose of them correctly. Do not throw them out in the regular rubbish bin! Put them in a sharps bin that is designed for needles.
It’s also important not to use anyone else’s insulin pens, even if the pen needle is changed. They might use a different kind of insulin. That also means that you shouldn’t let anyone else use your insulin pen either!
Continuous subcutaneous insulin infusion (aka insulin pump)
Continuous subcutaneous insulin infusion is more commonly referred to as an insulin pump. These pumps store rapid-acting insulin in the cartridge. Basal insulin is supplied through continuous infusion and a pre-meal bolus is set by the wearer and depends on the carbohydrate content of the meal.
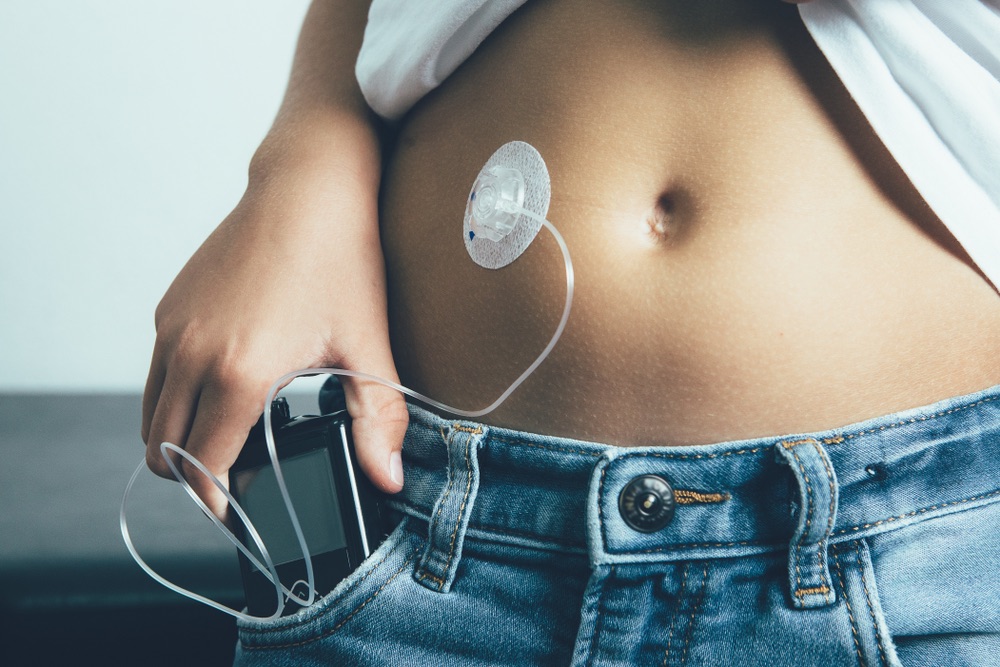
How do insulin pumps work?
The insulin pumps work by slowly delivery insulin into the body. This is a small dose of insulin every few minutes all throughout the day and night. This is the basal insulin dose. The insulin travels through a thin tube (as thin as spaghetti!), with one end connected to the pump and the other end inserted through an opening in the skin. These pumps are designed to work all day and night!
The catheter, which is what is inserted into the skin, should be taken out and re-inserted approximately every 2-3 days. Your doctor will teach you how to do this. It’s a relatively quick and painless.
Insulin pumps and continuous glucose monitoring
Continuous glucose monitoring (CGM) used with an insulin pump can alert a user to fluctuations in blood glucose levels with alarms and visual displays on the pump itself. This combination can give a user more information about their blood glucose levels.
There are some insulin pumps that can automatically adjust the basal insulin dose depending on the CGM results, acting like an artificial pancreas!
To learn more, read our article about low glucose suspend and how insulin pumps are able to act like a pancreas!
How often should I use insulin every day?
The amount of insulin that you use every day will depend. Your doctor will be able to help you work out a treatment plan. Your doctor will be also be able to help you decide which insulin delivery method works best for you and your lifestyle. A treatment plan can tell you:
- what type of insulin to use
- when to use insulin
- how much insulin to use
How much insulin should I use every day?
What you do throughout our day can influence how much insulin you use. This includes what you eat and how physically active you are. When choosing how much insulin to use, you will need to think about the following:
- what the next meal will be
- if there is any planned exercise or physical activity
- what the current blood glucose levels are
There are other factors that can change how much insulin a person uses. These include:
- having surgery, getting sick, are pregnant
- eating out
- travelling
- gaining or losing weight
Do I need to keep checking my blood glucose levels?
Yes. It’s important to keep checking your blood glucose levels for a number of important reasons. Checking your blood glucose can tell you:
- If your glucose levels are too high or too low – If you use too much insulin, it can cause your blood glucose levels to become too low. If you don’t use enough insulin, then your blood glucose levels can become too high. If your blood glucose levels become too low or too high, then it can cause some serious problems.
- How well your treatment is working – The goal of diabetes treatment is to keep blood glucose levels as close to or at a normal level. Ongoing high blood glucose levels can lead to diabetes-related complications later in life.
- What changes to make at next insulin dose – Knowing what your blood glucose levels are, will help you to work out how much insulin to use at your next dose.
How do I check my blood glucose levels?
You can monitor blood glucose levels by self-monitoring with a glucose meter or continuous glucose monitoring.
Self-monitoring with a glucose meter involves testing a small drop of blood, often drawn from the finger-tip with a lancet. While continuous glucose monitoring can transmit blood glucose levels every five minutes, through a sensor typically inserted into the back of the arm.
What are the recommended Hb A1c target ranges for patients with diabetes?
For some patients, their doctor may provide them with their own personalised Hb A1c target range. There are general target ranges, as well as target ranges depending on other factors like age (child vs adult) or pregnancy.
Recommended Hb A1c target ranges for patients with type 1 diabetes
| Hb A1c Target | |
|---|---|
| General | <7.0% - <53 mmol/mol |
| Pregnancy or planning pregnancy | <7.0% - <53 mmol/mol |
| Children and adolescents | <7.5% - <58 mmol/mol |
What should I do next?
If you experience any symptoms of type 1 diabetes or you have risk factors for developing type 1 diabetes, it is important to get tested for as soon as possible. Some people are at higher risk and need regular testing.
By diagnosing and treating the type 1 diabetes early, it means you can decrease the risk of developing or delay any further health complications of type 1 diabetes, for example nerve damage, blindness, and heart disease. It is important to know that diagnosing type 1 diabetes should not rely solely on using a Hb A1c test.
Once you learn what your type 1 diagnosis is, or if you already have type 1 diabetes, the next most important step is to become educated. You can join the 12-week Type 1 Diabetes Program to help you learn how best to manage the condition. For example, you can learn how best to monitor blood glucose levels in type 1 diabetes. The program is personalised and tailored, giving you more of the content that you want. The program also helps you to stay motivated and teaches you what changes you need to make. The first week is free and full of helpful and crucial information.
Interested in more information on type 1 diabetes?
Follow the links below to learn more about type 1 diabetes.