Monitoring your health when you have gestational diabetes is vital for mum and baby
Medically reviewed by Dr Sultan Linjawi, Endocrinologist & Diabetes Specialist — December 2025
What is gestational diabetes?
In pregnancy there many hormonal changes that occur in the mother in order to facilitate the growth of a baby. Many of these changes are caused by hormones produced by the placenta. Some of these hormones cause the mother’s insulin receptors to become resistant to insulin. Insulin is a chemical that acts like a key, and when bound to the insulin receptor on a cell surface, opens a lock or channel so that glucose can move from the blood into the cells.
Gestational Diabetes Content |
|---|
| Gestational Diabetes Program |
| Overview |
| Risk Factors |
| Symptoms |
| Diagnosis |
| Complications |
| Treatment |
| Diet |
| Monitoring |
| Tools |
| Mental Health |
| Prevention |
As the placenta grows during the pregnancy, more and more hormones are made and released to support the growth of the baby. This makes the mother more and more insulin resistant. At some point the mother may not be able to produce enough insulin to overcome the resistance, and if this occurs blood glucose levels rise.
Monitoring blood glucose levels at home
You may be checking and monitoring your blood glucose levels around four times per day, or even more if you’re using insulin. Careful and regular daily monitoring is the only way to ensure that your blood glucose levels remain within the target range. If you have type 2 diabetes and you aren’t using insulin, you will likely check your blood glucose levels less frequently throughout the day.
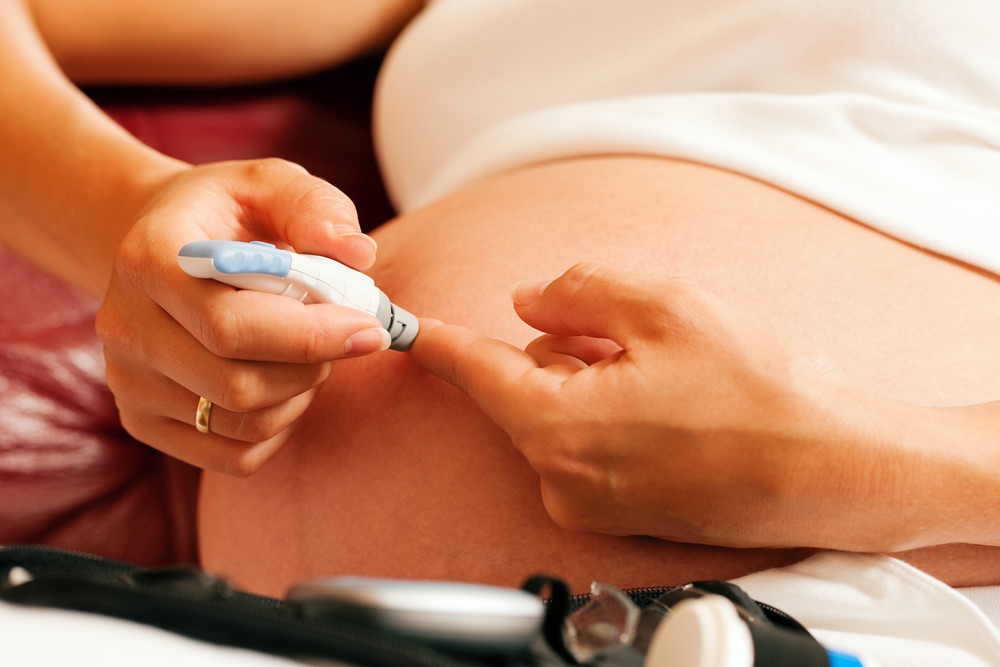
Testing blood glucose levels with fingersticks and a glucose meter?
When testing your blood glucose levels through a finger prick test, it’s important to follow the directions of your doctor or the instructions on the glucose meter. It’s important never to share glucose monitoring equipment, as this can lead to infection.
Some general guidelines for testing blood glucose levels include:
- Wash hands with soap and warm water, then dry thoroughly.
- Prepare the lancet device, using a fresh lancet. The lancet will help to draw a small amount of blood from your finger.
- Prepare the glucose meter and test strip.
- Use the lancet to draw a small drop of blood from your finger tip.
- Apply the drop of blood to the test strip in the glucose meter. The result will appear on the display on the meter after several seconds.
- Dispose the lancet in a sharps bin (not in your regular household bin).
How accurate is home testing with blood glucose meters?
Blood glucose meters are reasonably accurate, however there can be some variability between different devices. You can check the accuracy of your meter by taking it with you to your doctor and testing your glucose levels with your machine at the same time as having a blood test. You can compare the results to check if there are any differences. If the results differ significantly, there might be something wrong with your machine and you need to get a new one!
How to prevent inaccurate results
Sometimes you might get a blood glucose result that doesn’t fit with how you feel. For example, you may get a reading that says your blood glucose levels are low, but you aren’t exhibiting any symptoms of hypoglycaemia. If this happens, take a second reading or try testing on an alternative glucose meter if you have access to one.
It’s also important to make sure that you wash your hands thoroughly and dry them before conducting the finger prick test. If you don’t wash your hands properly after eating and before testing, you may contaminate the results. This can occur because of any food residue or crumbs left on your fingers, could provide a falsely high reading.
If you don’t dry your hands thoroughly after washing them, then you may get a falsely lowered blood glucose reading! Any water left on your finger may dilute your blood when you’re testing your glucose levels.
You can also prevent inaccurate results by doing the following:
- Ensure test strips aren’t expired
- Ensure the test strips ‘match’ the glucose meter – some glucose meters have specific test strips
- Draw enough blood for the test strip
- Don’t let the test strip with the blood drop dry before putting it in the glucose meter – insert the strip right away
- Keep the glucose meter clean by storing the meter in a clean dry area to avoid dust getting on the sensor
- Keep the battery fully charged
Let's enter your
Fasting Blood Sugar Level
mg/dl
Does gestational diabetes go away after delivery?
Generally, most cases of gestational diabetes disappear after pregnancy. This however does need to be confirmed 6-10 weeks after delivery with another 2-hour glucose tolerance test.
50% of mothers with gestational diabetes will go on to develop type 2 diabetes later in life and this is more likely to occur if the correct lifestyle changes are not undertaken. If a mother with previous gestational diabetes becomes pregnant again then the next pregnancy should always be considered high risk for subsequent diabetes and be tested for early in pregnancy.
Monitoring for diabetes after pregnancy
Approximately 6-10 weeks post-pregnancy, all women should be tested for type 2 diabetes. This is again through an oral glucose tolerance test (OGTT), which requires you to fast for at least 8 hours, have two blood tests, and consume a syrupy glucose solution. If the blood glucose results come back within the normal range then you don’t have type 2 diabetes, however you are still at a high risk of developing diabetes. You need to continue to be tested every two years through an OGTT.
What should I do next?
If you experience any symptoms of gestational diabetes or you have risk factors for developing gestational diabetes, it is important to be tested at 24-28 weeks gestation. Some people are at higher risk than others. If you are 25 years or older or have other risk factors for diabetes, you may require testing earlier in pregnancy. By diagnosing and treating gestational diabetes, it means you can decrease the risk of developing or delay any further health complications of gestational diabetes. These complications can affect both you and your child later in life, for example you are both at risk of developing type 2 diabetes. It is important to know that diagnosing diabetes should not rely solely on using a Hb A1c test.
Once you learn what your gestational diabetes status is, or if you already have gestational diabetes, the next most important step is to become educated. You can join the Gestational Diabetes Program to help you learn how to manage gestational diabetes and improve health outcomes for you and your child. The program is personalised and tailored, giving you more of the content that you want. The program also helps you to stay motivated and teaches you what changes you need to make.
Interested in more information on gestational diabetes and diabetes in pregnancy?
Follow the links below to learn more about gestational diabetes.



